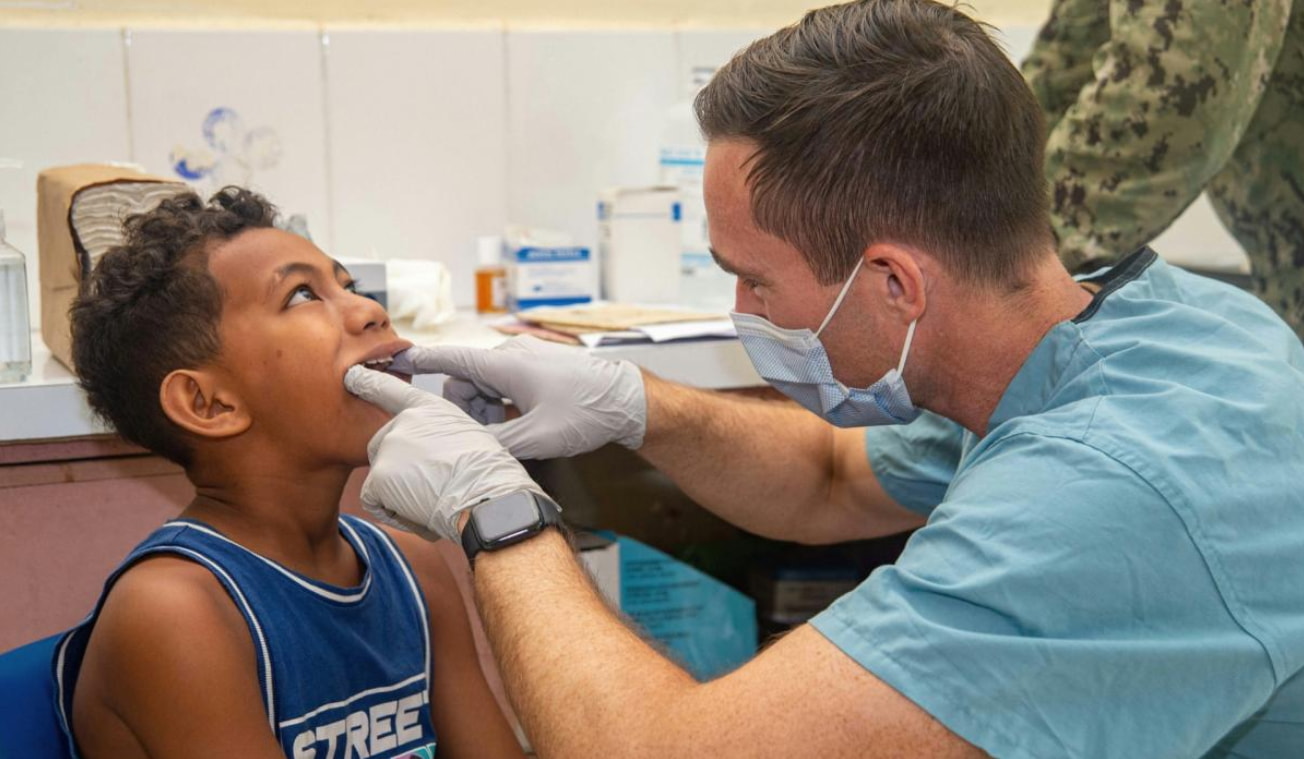
The center isn’t the only healthcare facility forced to shut down. Motherly reports that rural towns across the U.S. are doomed to the same fate. Sweeping federal Medicaid cuts are disproportionately threatening rural hospitals, leaving the healthcare gap even wider.
Access to healthcare is a basic human right, and should not depend on your postcode. For millions of people living in rural areas, it still does. Clinics are far apart. Hospitals close. Specialists stay in cities. The result? Longer travel, delayed care, and poorer health outcomes.
Thankfully, people are stepping up. Communities, new technologies, migrant professionals, and advanced practice nurses are all helping fill the cracks. It’s not perfect. Yet it shows what happens when healthcare is treated as an inclusive public service.
Why Rural Healthcare Gaps Exist
Distance and Workforce Shortages
It’s a given that most rural residents live far from hospitals or specialists. Transportation
can be unreliable. Costs add up quickly.
The Rural Health Information Hub states that geographic isolation and workforce shortages remain two of the biggest barriers to care in rural communities. Unfortunately, healthcare workers tend to cluster in areas with higher pay and better resources. Cities win that competition most of the time.
Economic Pressure on Rural Hospitals
Small hospitals operate on thin margins. When funding drops, closures follow. That leaves entire regions scrambling for alternatives.
The American Heart Association highlights how these closures affect emergency response, chronic disease care, and preventative services. That’s not merely inconvenient; it’s life-threatening.
Advanced Practice Nurses Filling Primary Care Gaps
The Growing Role of Family Nurse Practitioners
Family Nurse Practitioners (FNPs) are increasingly central in underserved areas. They provide primary care, chronic disease management, and preventative services.
Many train through flexible programs, such as FNP nursing programs online. Some may have started as registered nurses (RNs) serving their communities, and taking the online option is the only viable choice.
Online family nurse practitioner programs help working nurses advance without leaving their communities. That matters. Local providers are more likely to stay local. Spring Arbor University says that online MSN-FNP programs are designed for nursing students who want to advance their skills and lead a fulfilling career.
Midwives Stepping in Too
As previously mentioned, rural maternal care has taken a hit in recent years. Midwives are helping stabilize services.
In New Mexico, they’ve filled essential maternity care roles where obstetric units closed. These nurses provide respectful care in a community that is most often underrepresented in data and research.
This approach is practical. It’s also community-centered. Patients prefer familiar faces who understand local culture.
Foreign Professionals Supporting Rural Systems
Healthcare migration is sometimes framed negatively. The reality is more nuanced.
Many immigrant doctors work where shortages are most severe. These physicians play a critical role in sustaining access to U.S. healthcare, particularly in underserved regions.
You might not know this, but nearly one quarter of physicians in the country are international medical graduates. That contribution deserves recognition. Healthcare works best when talent moves where it’s needed most.
Community-Based Care Models
Care Rooted in Local Relationships
Some programs focus less on big hospitals and more on grassroots care. Institutions have created initiatives where healthcare providers collaborate closely with local communities to deliver culturally relevant services.
This model builds trust. And trust improves outcomes.
Public Health Approaches Gaining Traction
Research published in Frontiers in Public Health points to community-driven strategies as key to improving rural health equity. They include outreach programs, preventative education, and shared decision-making.
It’s less top-down and more collaborative.
Digital Health Is Changing the Game
Telehealth and Remote Monitoring
Telemedicine has expanded in recent years. It reduces travel time and increases access to specialists.
A study published on Cureus on digital healthcare infrastructure shows how telehealth strengthens care delivery in remote areas. Still, internet connectivity remains uneven.
Digital equity is now also a health equity issue.
Mobile Health Innovations Globally
Innovation isn’t limited to wealthy countries. In Ghana, a mobile health app is helping bridge rural care gaps by connecting patients with services and health education.
Solutions don’t always require massive budgets. Sometimes they require smart design and community input.
The Bigger Picture: Healthcare as a Collective Responsibility
Equitable access to healthcare is political. A lack of service often reflects broader inequality. Rural areas frequently receive less investment. That shapes everything from infrastructure to education to medical services.
A more collective approach can help. Training local providers. Supporting immigrant clinicians. Funding community clinics. Expanding telehealth access. These steps emphasize care over profit.
That perspective isn’t radical; it’s pragmatic because healthy communities benefit everyone.